Why Some Physicians are Opting Out of Meaningful Use Attestation
By Charles Settles
Since its inception, the Meaningful Use Incentive Program (MUIP) has paid out nearly $30 billion worth of incentives, but a rising number of physicians are opting out. Why?
2011, the first year of the MUIP, saw widespread interest. Nearly 200,000 eligible providers (EPs) and over 3,000 hospitals completed registration for either the Medicare or Medicaid versions of the program, according to the latest summary report from CMS. However, much of this original momentum appears to be lost. 2014 saw under 73,000 EPs and just 108 hospitals register across both programs.
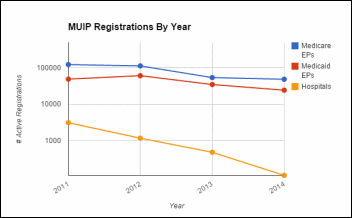
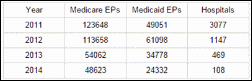
Altogether, 515,158 registrations have been completed by EPs across both programs, with 415,550 unique EPs receiving an average of $25,190 in incentive payments. According to the CMS’s latest data, just over half of eligible providers have received an incentive payment. But what about the other (at least) 40 percent?
It can’t simply be a question of eligibility. According to Medscape’s 2014 EHR Report, only 22 percent of physicians are abandoning or have never supported the MUIP, but examining the CMS summary report suggests a much higher rate of attrition — only 23 percent of the 260,900 physician EPs who received a payment in 2013 received one in 2014. That translates to an attrition rate of just under 77 percent.
When considering the payments only by stage of the program, the numbers for physicians are even worse — only 5.7 percent of those physicians who received a payment for the first stage have received one for the second. More physicians will complete Stage 2 eventually, but the odds of making it to CMS’s 75 percent adoption rate target by 2018 appear to be growing shorter. The carrot simply hasn’t been enough.
The stick may not be enough either. If the 75 percent adoption rate target is not met, reimbursements stand to be cut by up to five percent. The average family physician, arguably the primary focus of the MUIP, receives about $100,000 per year from Medicare reimbursements, according to Dr. Jason Mitchell, former director of the American Academy of Family Physicians’ Center for Health IT. Since the penalties increase by one percent per year beginning with a one percent penalty in 2015, a physician receiving $100,000 annually could lose up to $10,000 in reimbursements through 2018. For some, the penalty is a small price to pay to not have to deal with requirements that they feel prevent them from delivering better patient care.
Dr. S. Steve Samudrala, medical director of America’s Family Doctors, was an early proponent of electronic health records, patient engagement, and other medical software systems. It seems ironic that Dr. Samudrala does not participate …read more





